Every healthcare provider delivers a service. But delivering that service and actually getting paid for it are two very different things. The process that connects those two points is called healthcare revenue cycle management. It covers everything from the moment a patient schedules an appointment to the moment the provider receives the final payment.
For any healthcare organization, understanding and managing this process well is the difference between financial stability and constant cash flow problems. A single weak point in the cycle can delay payments for weeks, trigger claim denials, and put real strain on operations.
This blog breaks down what the revenue cycle actually involves, where most practices run into trouble, and what it takes to manage it well.
Understanding Healthcare Revenue Cycle Management for Practices
Healthcare revenue cycle management is the complete financial process that healthcare providers use to manage patient service revenue. It begins at patient registration and ends when all payments have been collected, and the account is closed.
The process includes patient registration, insurance eligibility verification, clinical documentation, medical coding, claim submission, payment posting, denial management, and patient balance collection. Each stage is connected to the next. A problem at any point creates downstream effects on the entire cycle.
Why Healthcare Revenue Cycle Management is Important for Medical Practices
Healthcare spending in the U.S. continues to climb. According to the Centers for Medicare & Medicaid Services, U.S. healthcare spending grew 7.2% in 2024, reaching $5.3 trillion, or about $15,474 per person, accounting for 18% of the nation’s GDP.
Poor revenue cycle performance doesn’t just hurt a practice’s bottom line but also creates delays in care, staff burnout, and patient frustration.
A strong healthcare revenue cycle management process means fewer denied claims, faster payment turnaround, and cleaner financial reporting. It also means patients understand their financial responsibility upfront, which leads to better collection rates and fewer billing surprises.
Key Stages of Healthcare Revenue Cycle Management (RCM)
Think of the revenue cycle as a chain. Break one link, and the whole thing slows down. Here’s how it typically flows:
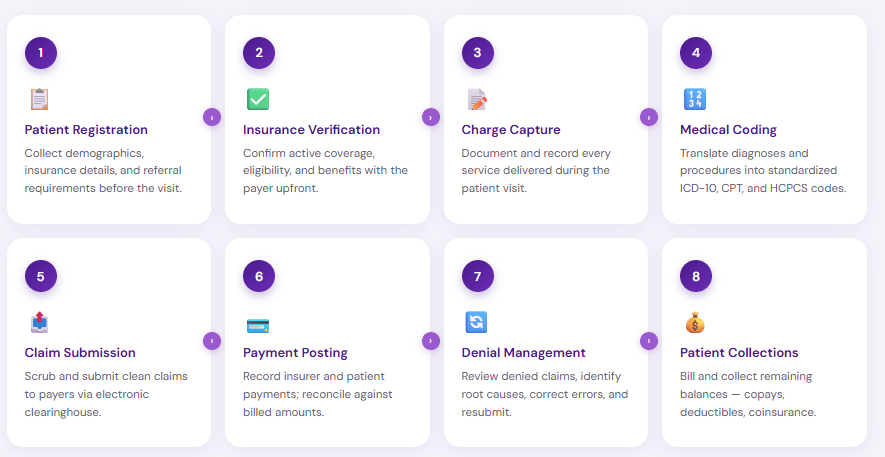
- Patient Registration and Insurance Verification
The revenue cycle begins before the patient arrives. At registration, staff collect the patient’s demographic information, insurance details, and any referral or authorization requirements. Insurance eligibility is verified to confirm active coverage and understand what the plan will and will not cover.
- Medical Coding
Once the provider completes the patient visit, clinical notes are translated into standardized billing codes. Diagnosis codes come from the ICD-10 system. Procedure codes come from the CPT and HCPCS systems. These codes tell the insurance payer exactly what condition was treated and what services were performed.
A mismatched code or a missing modifier can result in an immediate claim denial. The American Academy of Professional Coders confirms that coding accuracy affects both reimbursement rates and compliance, making it one of the most important skills in any billing team.
- Claim Submission and Scrubbing
After coding, the claim is submitted to the payer, usually through an electronic clearinghouse. Before submission, the claim goes through a scrubbing process that checks for errors, missing fields, and code mismatches. Clean claims pass through quickly. Problematic claims get flagged for correction before they ever reach the payer.
- Denial Management
Not all claims are paid on the first submission. Payers deny claims for many reasons, including incorrect codes, missing prior authorizations, coordination of benefits issues, and eligibility problems. The industry average denial rate is between 5 and 10%, though some practices see rates closer to 20%. Managing denials means reviewing each one, identifying the root cause, correcting the error, and resubmitting before the filing deadline.
- Payment Posting and Patient Collections
When payments arrive from payers, they are posted to the correct patient accounts and reconciled against what was billed. Any remaining balance after insurance payment becomes the patient’s responsibility in the form of copays, deductibles, or coinsurance.
Collecting patient balances has become a larger part of the revenue cycle over the past several years. High-deductible health plans have shifted more financial responsibility to patients, which means practices now spend more time and resources on patient collection strategies than they did a decade ago.
The Flow of the Healthcare Revenue Cycle
| RCM Stage | What Happens | Why It Matters |
| Patient Registration | Patient details, insurance information, and demographics are collected. | Accurate information prevents billing errors and claim rejections. |
| Insurance Verification | The practice confirms coverage, eligibility, and benefits with the payer. | Reduces claim denials and unexpected patient costs. |
| Charge Capture | All services provided during the visit are documented and recorded. | Ensures the practice bills for every service delivered. |
| Medical Coding | Diagnoses and procedures are translated into standardized codes. | Accurate coding helps claims get approved faster. |
| Claim Submission | Claims are submitted to insurance companies for reimbursement. | Timely submission speeds up the payment process. |
| Payment Posting | Payments from insurers and patients are recorded in the system. | Keeps financial records accurate and updated. |
| Denial Management | Denied or rejected claims are reviewed, corrected, and resubmitted. | Helps recover revenue that would otherwise be lost. |
| Patient Billing & Collections | Patients receive bills for their remaining balance and make payments. | Ensures the practice collects the full amount owed. |
Final Thoughts
Healthcare revenue cycle management is the financial backbone of every healthcare organization. When the process runs well, providers get paid accurately and on time, staff spend their energy on productive work, and patients have a clear understanding of what they owe. When the process breaks down, the effects reach well beyond billing. Delayed payments affect staffing decisions, technology investments, and the ability to deliver quality care.
For many practices, managing these improvements internally can be challenging without the right expertise or resources. That is where Elite MedBilling Solutions and Revenue Management can help. Their team works with healthcare practices to identify revenue leaks, reduce denials, and streamline billing workflows, helping providers strengthen their revenue cycle while focusing more on patient care.
FAQs
1. What is healthcare revenue cycle management in simple terms?
It is the complete process a healthcare provider uses to bill for services and collect payment. It covers everything from verifying a patient’s insurance before a visit to posting the final payment after the claim has been processed.
2. What is the difference between medical billing and revenue cycle management?
Medical billing refers specifically to the process of submitting and following up on claims. Revenue cycle management is broader. It includes billing, but also covers patient registration, eligibility verification, coding, denial management, and patient collections. Billing is one piece of the overall revenue cycle.
3. What is a clean claim rate, and why does it matter?
A clean claim rate measures the percentage of claims accepted by a payer on the first submission without errors. A rate above 95% is generally considered strong. A lower rate means more claims are being rejected, which leads to rework, payment delays, and increased administrative costs.
4. How does prior authorization affect the revenue cycle?
Prior authorization is required by many payers before certain services are performed. If a provider delivers a service without the required authorization, the payer can deny the claim entirely. Tracking authorization requirements by payer and service type is a basic but important part of keeping the revenue cycle clean.
5. What does Days in Accounts Receivable mean?
Days in Accounts Receivable (Days in AR) measures the average number of days it takes a practice to collect payment after a service is billed. A benchmark below 35 to 40 days is generally healthy. A rising number indicates a slowdown somewhere in the billing or collections process that needs to be investigated.